Frattura dello scafoide
- Home
- Injuries and Pathologies of the Elbow, Wrist and Hand
- Scaphoid fracture
The scaphoid fractures are the most frequent among those of carpal bones (almost 90% of the total). They usually occur as a result of a hyperextensional fall in the hand and may be associated with lesions of the small ligaments surrounding the scaphoid and stabilizing it with the other bones, particularly the lunate bone.
In general, the fracture produces severe pain and a often significant swelling localized near the anatomic snuffbox (that small triangular area at the base of the thumb). Pain limits movements on all floors.
For simplicity we consider 3 types of fractures: proximal, distal and isthmic.
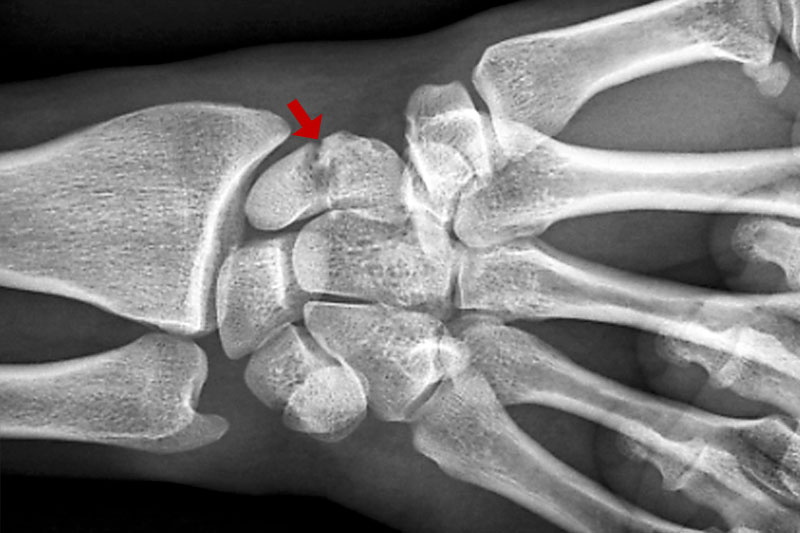
Localization significantly influences the therapeutic choice and the long-term prognosis. In summary, fractures with longer healing times and more at risk of complications are proximal because the blood supply occurs in the distal-proximal direction; indeed, a clear superiority of vascularization at 2/3 distal with respect to the proximal third is demonstrated.
The doctor to make a diagnosis is based on the medical history and the clinic; in general the diagnosis of the doctor is confirmed by a radiograph of the wrist in particular projections for the scaphoid. Sometimes a fracture can go unnoticed at a first X-ray examination; if the clinical suspicion persists, it is advisable to repeat the radiographic examination after 15 days or immediately perform a CT scan to confirm the diagnosis.
A late diagnosis or a too short immobilization are the most frequent causes of complications such as osteonecrosis of the proximal pole and pseudoarthrosis.
The treatment is generally conservative and consists of packaging a plaster with an included thumb to hold 6 -10 weeks. Instead, proximal fractures are treated surgically with osteosynthesis through a small cannulated screw (Herbert’s screw) and immobilization with a brace for about 2 weeks.
To remove the plaster or the brace (which occurs after radiological healing) it is advisable to start a cycle of rehabilitative therapies aimed at recovering the articularity and strength of the intrinsic and extrinsic musculature of the hand. The therapeutic program is completed with specific occupational therapy exercises and recovery of sports technical gestures.
Scaphoid fracture – Rehabilitation
The typical mechanism of fracture of the scaphoid is the fall on a pose hand in hyperextension for wedging the scaphoid against the dorsal edge of the radius. There is always a surgical indication with plaster cast for 6/10 weeks application (not more than 3 months). The functional recovery is not possible without a personalized rehabilitation program.
The first goal of rehabilitation is the recovery of the physiological ROM (usually very small) through passive and active mobilizations in flexion, extension, pronation and supination of the wrist, interphalangeal joint mobilization of both the thumb of the adjacent fingers. In this phase, physical therapies (ice, laser, ultrasonic immersion) and massotherapy draining and upper limb relaxant are useful to control pain.
After reaching the full range of motion it is possible to progress to the second phase of rehabilitation that focuses on the recovery of the strength of epicondylus and epitrochlear muscles with exercises against manual resistance and weights and on the recovery of the trophism of the intrinsic muscles of the hand with rubber bands, balls of different consistencies, pliers and retinas.
The rehabilitation program ends with the last phase on the sports field with proprioceptive exercises for neuromotor recovery of hand function and others that bring the patient to perform sports specific gestures to launch exercises/gripping objects and push ups on unstable surfaces for prevention of falls.


